The maternal mortality rate in America is a lot higher than you think. And what’s worse is that the complications that some mothers experience are easily preventable. There needs to be better care for mothers, especially in a nation advanced as America.
Leah Bahrencu’s kidneys and liver shut down.
Samantha Blackwell spent a month in a coma.
Cindel Pena suffered heart failure.
Heather Lavender lost her uterus.
Rebecca Derohanian bled into her brain.
Every year in the U.S., nearly 4 million women give birth, the vast majority without anything going amiss for themselves or their babies. But more than 135 expectant and new mothers a day — or more than 50,000 a year, according to the Centers for Disease Control and Prevention — endure dangerous and even life-threatening complications that often leave them wounded, weakened, traumatized, financially devastated, unable to bear more children or searching in vain for answers about what went wrong.
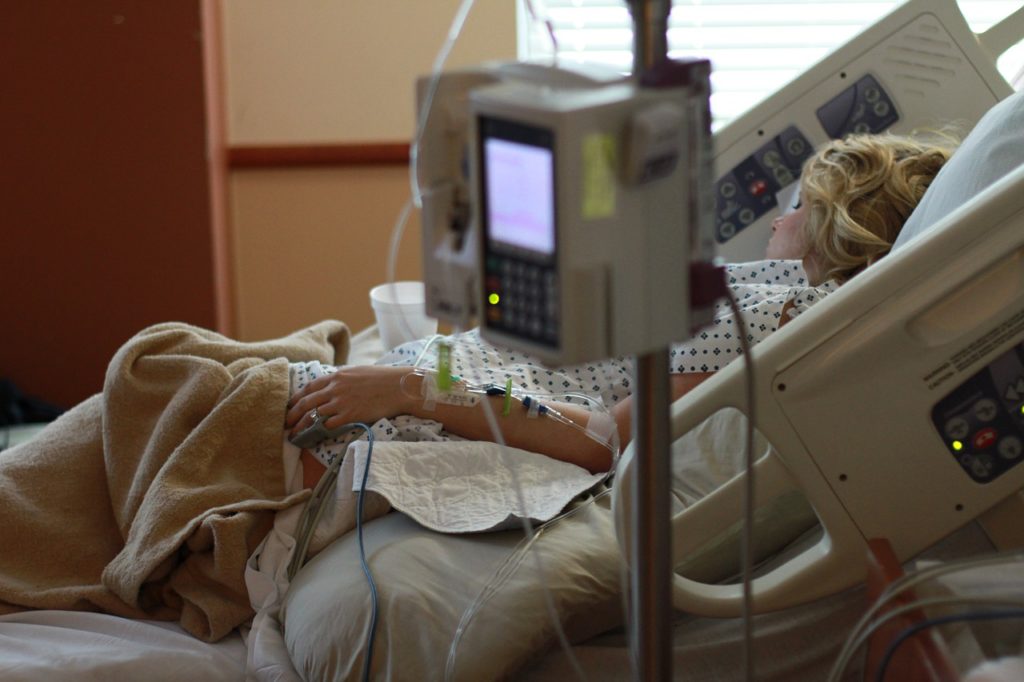
For the past year, ProPublica and NPR have been examining why the U.S. has the highest rate of maternal mortality in the industrialized world. The 700 to 900 deaths each year related to pregnancy and childbirth, though, overshadow a more pervasive problem that experts call “severe maternal morbidity.” For every U.S. woman who dies as a consequence of pregnancy or childbirth, up to 70 suffer hemorrhages, organ failure or other significant complications, amounting to more than 1 percent of all births. The annual cost to women, their families, taxpayers and the health care system runs into billions of dollars.
“There’s this misconception that these complications are rare,” said Kristen Terlizzi, cofounder of the National Accreta Foundation, who had her uterus, appendix and part of her bladder removed in 2014 because of a life-threatening placenta condition, “and we [women] get brushed off — ‘The risk is not a big deal.’ But it is.”
Better care could have prevented or alleviated many of these complications, experts say. Maternal morbidity encompasses a spectrum of problems, from moderately serious to near-deadly, and proper medical attention can stop treatable conditions from spiraling out of control. In a 2016 study of all women admitted for delivery over 30 months at Cedars-Sinai Medical Center in Los Angeles, California, researchers found “opportunity for improvement in care” in 44 percent of life-threatening complications related to pregnancy and childbirth.
What’s more, according to the CDC, severe maternal morbidity has risen faster than maternal mortality. Based on the rate per 10,000 deliveries, serious complications more than doubled from 1993 to 2014, driven largely by a five-fold rise in blood transfusions. That also includes a nearly 60 percent rise in emergency hysterectomies — removal of the uterus and sometimes other reproductive organs, often to stem massive bleeding or infection. In 2014 alone, more than 4,000 women had emergency hysterectomies, rendering them permanently unable to carry a child. The rates of new mothers requiring breathing tubes, and of treatment for sepsis — a life-threatening inflammatory response to infection that can damage tissues and organs — both increased by 75 percent. And the rate of women needing to be resuscitated from heart failure rose by 175 percent, to a total of roughly 400.
“These numbers are really high, and far too many of them are preventable,” said Dr. Elliott Main, medical director of the California Maternal Quality Care Collaborativeand a national leader in efforts to reduce maternal deaths and injuries.
Judged by one of the most life-altering impacts — a hysterectomy — the U.S. is an outlier in the industrialized world. U.S. women are about five times more likely than their British and Swedish counterparts to undergo a hysterectomy, according to Elena Kuklina, a CDC health scientist. They’re also three times more likely to need a breathing tube during and immediately after childbirth than women in the United Kingdom. The U.K. has improved maternity care by requiring every doctor to follow the same treatment protocols, and by examining every death to see what mistakes may have occurred.
While hospital and government authorities in the U.S. often fail to investigate why a new mother died, complications that aren’t fatal receive even less scrutiny. More than 30 states and cities now have committees to review maternal deaths, but only one state — Illinois — has started to systematically examine severe complications. (That process, which began July 1, so far only has funding for one year.) New York City’s committee, which met for the first time this month, plans to look at both deaths and severe complications. The Joint Commission, the not-for-profit body that accredits health care facilities, requires hospitals to do a thorough analysis of severe morbidity (whether involving new mothers or any other patients) only when a complication is “not primarily related” to the “natural course of the patient’s illness or underlying condition.”
More scrutiny of near-deaths could illuminate not only what went wrong but what went right. “Maybe everything was done really, really well, and they saved the woman’s life,” said Stacie Geller, a maternal health expert who directs the Center for Research on Women and Gender at the University of Illinois at Chicago.
The U.S. government, which stopped publishing an official annual count of pregnancy-related fatalities a decade ago, has had similar difficulties tallying harm that doesn’t lead to death. After analysts fixed a computer programming error that had inflated the total, the CDC reduced its estimate of cases of “severe maternal morbidity” this year from 65,000 to more than 50,000. But its current number may be an undercount. Indeed, when one patient safety group, the Alliance for Innovation on Maternal Health (AIM), analyzed 2015 data from hospitals in four states, the rate of morbidity was roughly 2 percent of births, which would translate to 80,000 cases a year nationwide.
The CDC’s estimate encompasses 21 outcomes, from relatively minor hemorrhages if they require a blood transfusion, to kidney or respiratory failure. But it comes from hospital billing data generated when a new mother is discharged, and sometimes misses complications — bleeding, blood clots, even heart attacks — that may arise in the hours, days and weeks after she goes home. Hospital readmissions for childbirth-related ailments are difficult for researchers to track.
“The nature of our system is to focus on these women while they’re pregnant,” said Eugene Declercq, a professor of community health services at Boston University School of Public Health. “And then if there are difficulties later, they get lost to the larger system that doesn’t particularly care about women’s health to a great degree unless they’re pregnant.”
Samantha Blackwell experienced those postpartum difficulties. Eleven days after giving birth to her son in August 2014, Blackwell, then 25, woke with a pain in her lower abdomen so sharp that she couldn’t stand up straight, she said. The 25-year-old graduate student in nonprofit administration went to an emergency room at a hospital outside Cleveland, Ohio, where she was diagnosed with a massive infection and septic shock. According to her medical records, doctors performed a procedure known as a D&C, removing 400 milliliters of unidentified, foul-smelling material from her uterus. But her condition rapidly deteriorated and she was flown to a larger hospital 15 miles away.
While she lay in a medically induced coma, surgeons performed an emergency hysterectomy. When she regained consciousness a month later, she overheard her mother talking with a doctor, which was how she learned that her uterus had been removed.
“I’d have a million more kids if I could,” she said. “I hadn’t known how much I would love being a mother before they put my son on my chest.”

Blackwell was one of more than 4,000 women who shared stories with ProPublica and NPR of mothers nearly dying in childbirth. She was also one of more than 400 women who said they’d had an emergency hysterectomy. The procedure can often stop bleeding and save lives, yet it also ends women’s hopes for more children and sometimes leads to early menopause.
“Angry and sad. I woke up to find out I no longer had a uterus,” wrote 40-year-old Alicia Nichols of Needham, Massachusetts, who works in a cosmetic surgery office. After she gave birth to her first child this past March, she began experiencing bouts of bleeding, and took an ambulance to a hospital emergency room, but a doctor there told her that her symptoms were normal and sent her home, according to medical records. When her daughter was about two months old, Nichols had another scary episode, and made another appointment with an OB-GYN.
She was getting off the elevator at the doctor’s office when she began to hemorrhage. According to her medical records, she lost almost half her volume of blood. A week after being sent home, she was hospitalized with a life-threatening complication of that surgery, blood clots in both lungs.
Nichols had gotten pregnant via in vitro fertilization, freezing the extra embryos in hopes of having more children. Rather than surrender those dreams, she’s considering hiring a surrogate to carry her embryos to term — at a cost that could exceed $80,000.
Childbirth is the leading reason that people go to hospitals, accounting for nearly 12 percent of all U.S. hospital stays in 2014. Unlike the average patient, expectant mothers tend to be relatively young and healthy, brimming with joyful anticipation.
“You expect what you see in the movies,” said Leah Bahrencu, who taught Pilates and cardio-kickboxing in Austin, Texas, before she became pregnant with twins at 34. “Like it’s just routine: Your water breaks and you go to the doctor, and somewhere between four to maybe 20-something hours later, you have these babies.”
Bahrencu’s pregnancy seemed to be on track until this past January, when she was in her 34th week. At a routine checkup, she was diagnosed with HELLP syndrome, a particularly dangerous variant of preeclampsia (pregnancy-induced hypertension), and rushed to the hospital for an emergency cesarean section.

She then developed an infection that led to 10 days in a medically assisted coma. Her lungs, kidney and liver shut down, and she suffered permanent damage to her pancreas. “We almost lost her three times,” said her OB-GYN, Dr. Catherine Browne, whose voice broke repeatedly as she recalled the case.
As with many women who contacted ProPublica and NPR, Bahrencu’s problems persisted long after she finally went home. Subsequent infections sent Bahrencu to the hospital three more times, Browne said. Bahrencu stopped working outside the home and has struggled to care for her premature babies. “Emotionally, I’m a wreck,” she said. “I’m overwhelmed, and have to force myself to get out of the house. If I could, I would stay in my room while the kids are in the other room.”
She isn’t alone. Even seemingly temporary complications of pregnancy and childbirth may have long-term impacts on women’s physical and mental health. Preeclampsia, for example, substantially increases risks of heart disease and stroke later in life, while the trauma of a complicated birth can have emotional repercussions. About 1,370 women reported after-effects such as stress and depression, including more than 730 who told us that their physical suffering led to symptoms of post-traumatic stress disorder, or PTSD, a potentially disabling and sometimes chronic condition more often associated with combat veterans than with new mothers. Such symptoms can typically include flashbacks, nightmares, memory problems and feelings of hopelessness.
Up to 6 percent of new mothers suffer from PTSD, due to childbirth complications and other factors such as prior trauma, according to Sharon Dekel, an assistant professor of psychology at Harvard Medical School. Six months after giving birth, survivors of emergency hysterectomies are nearly 2.5 times more likely to have PTSD symptoms than women who didn’t have the surgery, according to a 2016 study.
“I’ve had dreams about being tied down … and feeling like I can’t breathe,” wrote a 36-year-old mother of two who teaches middle school in Manhasset, New York. She said she needed two surgeries and four pints of blood to stop a hemorrhage after an emergency C-section. “I was crying for a month after it happened,” she said.
“I feel like I can’t be without another adult with me at all times because I’m afraid of something happening to me and my baby will be alone. I constantly feel like I’m in survival mode,” wrote a 35-year-old stay-at-home mother of three in Traveler’s Rest, South Carolina, who said she survived a postpartum heart attack.
Read the rest of the article on Propublica.
By: Nina Martin, Propublica. Renee Montagne, NPR.

